Why does it burn “down there”?
A ring of fire. That’s what it can feel like.
You have pain with inserting a tampon. You’ve always dreaded pelvic exams because they hurt. Every time you try to have sex it burns and stings. Sound familiar? Pain with sex may be due to a lot of reasons – one of those may be vulvodynia.
A bit of history – pain with sex has always been an issue, but the cause has not always been well-known. It’s really only the past 20-30 years that our current understanding of it as a condition has been truly recognized, labeled, studied and appropriately treated. Knowing the true cause of the burning is critical in successfully treating it.
Side note:
For pain that you feel beyond the inner “lips” of the vulva, it’s likely tied to other conditions (ie, orthopedic issue, pudendal neuralgia, PGAD, etc). The reason for this distinction is because the skin right around the urethra and vagina is physiologically different from that found in the labia minora (inner lip) and beyond.
Similarly, certain dermatologic conditions can cause burning at or around the vestibule (ie lichen sclerosus, lichen planus, shingles, etc). These require good medical management along with physical therapy treatment of underlying muscle tension to be effectively treated.
These conditions deserve their own time and are beyond the scope of this blog. Let’s focus on pain that is local to / only in the vestibule today.
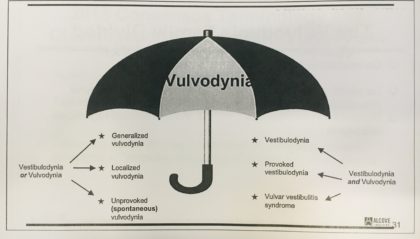
There are a lot of potential causes for burning or a sharp sensations. If the burning is in the urethra and/or vaginal opening region (ie, the “vestibule”), without any pain outside the ‘lips’ of the vulva, the vulvodynia is more appropriately called “vestibulodynia”.“Vestibulodynia” translates to “pain in the vestibule”. However, there are specific types of vulvar/vestibule pain and with those types come specific causes and therefore specific treatments.
This is is one of 7 different varieties of crotch anatomy that come in various colors, labels, and black & white that can be purchased to use for education at www.heatheredwardscreations.com
For some, burning around the vagina or urethra has always been there. This is called primary or congenital vulvodynia and is why you’ve never been able to use a tampon, have a pelvic exam or tolerate any touch in that area.
For others, the burning is a new thing. Maybe tampons and exams were fine. Sex may even have been fine for months or years – until it wasn’t. In that case, it may be acquired vulvodynia and it can be present in either ‘provoked’ (only with touch/insertion) or ‘non-provoked’ (there all the time) states.
Image Courtesy of Alcove Education
The most current research indicates four potential paths to acquired vulvodynia:
- Hormonal – altered response of the hormonal receptors in the area that leads to dryness, irritation, and thinning.
- Neuroproliferative – increase in the number of nerve endings in the area, causing it to become more sensitized.
- Inflammatory – local inflammation due to infection, medication or external agent irritation.
- Muscloskeletal – tension in the pelvic muscles, also known as Pelvic Floor Muscle Dysfunction (PFMD).
There is an amazing resource for those trying to understand more of this condition: Vulvodynia.com – It provides a chart and publications reviewing the differential diagnosis and recommended treatments. Note that there can also be, and often are, overlapping components of each of these categories.
Where does the musculoskeletal version of vestibulodynia come from? Pelvic floor muscle dysfunction can occur for a variety of reasons including in response to trauma, surgery, childbirth, inflammation, sexual abuse, or anxiety. Once the muscle tension occurs, it can drive neuropathic upregulation. In other words, the area becomes more sensitive and/or painful.
For those with vestibulodynia driven from musculoskeletal factors, physical therapy is one of the main treatment mechanisms. In addition to physical therapy interventions, some combination of other interventions may be indicated (yoga, cognitive behavioral therapy, vaginal diazepam, botox injections).
All of the treatments, including physical therapy, will be tailored to your particular situation but may include some version of the following:
- Manual treatments – External and/or internal hands-on techniques to reduce muscular or connective tissue restrictions in the area.
- Neuro Re-ed – Retraining of the muscles and nerves of the region to communicate effectively. This may be through Redcord training, biofeedback, or other mechanisms.
- Exercises – Of course physical therapy will involve some kind of exercise! The right exercise is important – sometimes retraining a muscle in how to relax is needed before strengthening can occur.
- Full body treatment – Let’s not ignore the rest of the body attached to this pelvis! Your PT will be able to evaluate all of the postural or mechanical issues that may be helping perpetuate tension through the pelvic region.
If you have questions regarding your pelvic pain, we can help you in determining your next steps.
References:
- Vulvodynia: Definition, Prevalence, Impact and Pathophysiological Factors. Pukall, C., Goldstein, A., et al. J Sex Med 2016;13:291-304.
- Recent advances in understanding provoked vestibulodynia. Lev-Sagie, A., Witkin, S. 2016.
- Polymorphisms of the Androgen Receptor Gene and Hormonal Contraceptive Induced Provoked Vestibulodynia. Goldstein, A., Belkin, Z., et al. J Sex Med 2014; 11:2764-2771.